What Is the Best Antibiotic for Bone Infection
Drainage from the area. 300 mg four times a day for 3 to 7 days.

Innovations In Osteomyelitis Research A Review Of Animal Models Roux 2021 Animal Models And Experimental Medicine Wiley Online Library
An additional course of oral antibiotics may be needed for more-serious infections.

. The drug may be delivered via injection at first and then continued for two weeks by the oral route. Each of these strategies focuses on a specific stage of the biofilm lifecycle. What are the best antibiotics for a foot infection.
Parallel-group randomised 1. Osteomyelitis is the infection and inflammation of the bone marrow. Fusidic acid is a bacterial protein synthesis inhibitor with antibiotic activity against.
However in case of less serious methicillin-susceptible Staphylococcus aureus or MSSA infections such as skin and soft. Overall most antibiotics including amoxicillin piperacillintazobactam cloxacillin cephalosporins carbapenems aztreonam aminoglycosides fluoroquinolones doxycycline vancomycin linezolid daptomycin clindamycin trimethoprimsulfamethoxazole fosfomycin rifampin dalbavancin and oritavancin showed good penetration into bone and joint tissues. Diabetes especially a diabetes-related foot ulcer.
An infection can start in a wound within a couple of days. It most frequently influences the bones of the extremities pelvis and spine. For managing the serious methicillin-susceptible Staphylococcus aureus or MSSA infections Penicillinase-resistant penicillins such as Flucloxacillin and dicloxacillin remain the antibiotics of choice.
This indicates that physicians select antibiotics empirically without culture information in about 60 of bone and joint infections. Based on the results in this study monotherapy with linezolid or TMPSMX and rifampin in combination with TMPSMX rather than fusidic acid or quinolone would be an appropriate treatment for patients with bone and joint. Such as Oxacillin Flucloxacillin First generation Cephalosporins.
500 mg four times a day for 3 to 7 days. Staphylococcus aureus bacteria staph infection typically cause osteomyelitis. The risk of infection is present until the wound heals.
Despite advances in both antibiotic and surgical treatment the long-term recurrence rate remains around 20. It can result from an infection somewhere else in the body that has spread to the bone or it can start in the bone often as a result of an injury. Boys are usually more affected.
If a wound looks or feels worse it is likely infected. Generally osteomyelitis of the jaws occurs when the. Complex bone and joint infections are typically managed with surgery and a prolonged course of treatment with intravenous antibiotic agents.
Antibiotic selection should provide good intracranial penetration and MDRSP coverage. The type of prescribed antibiotic will depend on the progression and severity of your infected foot. Research has to go further by finding specific antibiofilm strategies adapted to the PJI site.
Skin around the wound is red or hot. With the high frequency of invasive resistant strains in mastoiditis initial therapy of intravenous vancomycin and ceftriaxone is most appropriate until results of the culture and sensitivity studies are available. Irritability or generally feeling unwell.
Management of bone and joint infection commonly includes 4-6 weeks of intravenous IV antibiotics but there is little evidence to suggest that oral PO therapy results in worse outcomes. To determine whether or not PO antibiotics are non-inferior to IV antibiotics in treating bone and joint infection. Wounds should look and feel better as time goes on.
Other common symptoms are. Though rare this condition can affect the temporomandibular joint or TMJ that can cause severe issues with the bones of the face and jaw. The International Center for Limb Lengthening is a leader in healing patients with bone and joint infections.
While the exact choice of antibiotic will depend on the clinical situation any history of allergies resistance etc the use of amoxicillin is considered to be the best option to start with. Specific symptoms of wound infection include. Click to see full answer.
Commonly prescribed Staph infection antibiotics can include but are not limited to. Swelling in the affected area. Osteomyelitis is inflammation or swelling that occurs in the bone.
Artificial joint such as a hip replacement. Redness in the infected area. 5 rows Penicillin and amoxicillin.
This is an update of a Cochrane review first published in 2009. 76 rows Drugs used to treat Bone infection. Metal implants in bone such as a screw.
Osteomyelitis is more common in younger children five and under but can happen at any age. Sometimes a fungus or other germ causes a bone infection. 12 The preference for intravenous antibiotics reflects.
The following list of medications are in some way. Several strategies exist in order to fight bacterial infections and more particularly bone biofilm-related infections 3. Patients with mild infections can be treated with oral antibiotics like cephalexin.
She has authored and published many papers. Loading dose 500 mg on day 1 followed by 250 mg for an additional 4 days. Chronic osteomyelitis is generally treated with antibiotics and surgical debridement but can persist intermittently for years with frequent therapeutic failure or relapse.
The antibiotics are usually administered through a vein in your arm for about six weeks. If you have a history of mild allergy to penicillin ampicillin or amoxicillin the ADA recommends. Blood infection or conditions like sickle cell anemia.
Janet Conway is an internationally-recognized expert specializing in the treatment of bone and joint infections and has saved lives and limbs of patients who have failed to heal elsewhere. Penicillin refers to a class of antibiotics that includes penicillin. A bone biopsy will reveal what type of germ is causing your infection so your doctor can choose an antibiotic that works well against that type of infection.
Stiffness or inability.

Diagnosis And Management Of Diabetic Foot Infections Ncbi Bookshelf
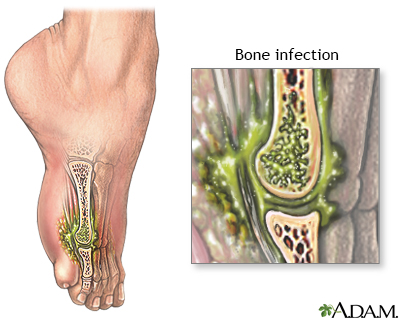
Osteomyelitis Information Mount Sinai New York
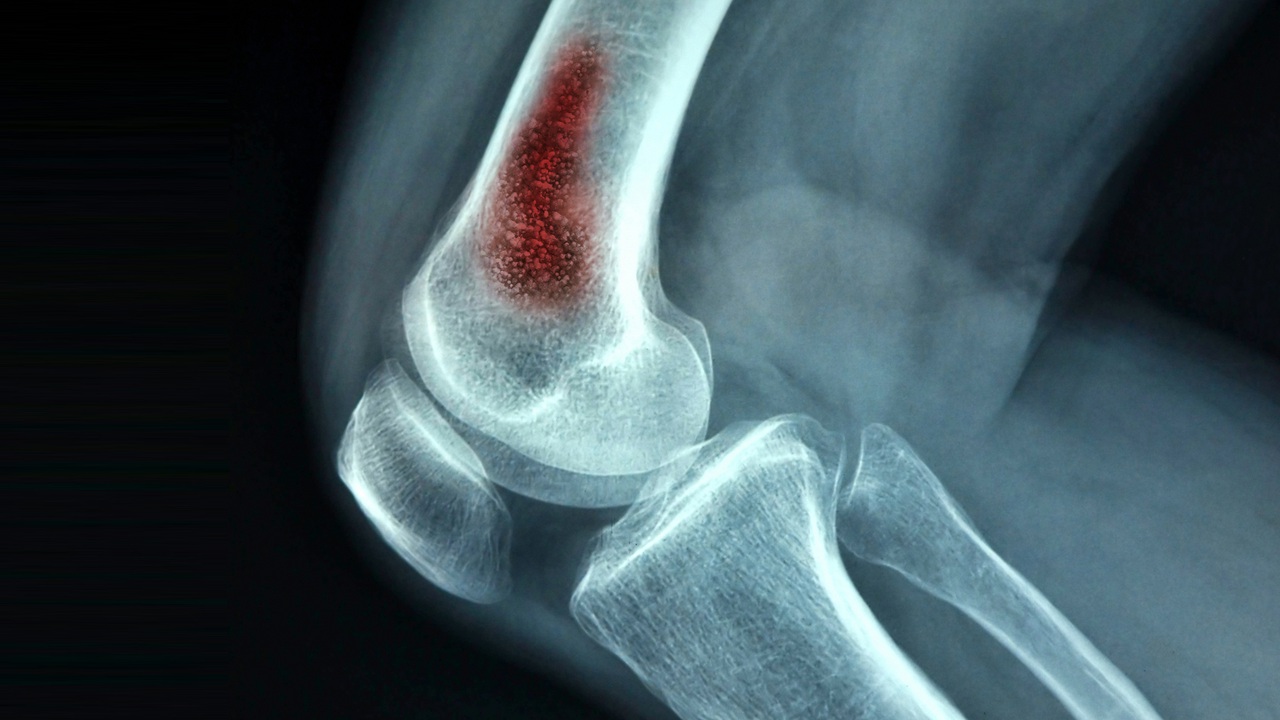
Osteomyelitis Johns Hopkins Medicine
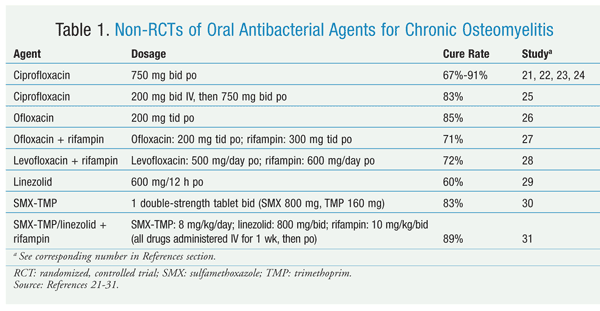
Oral Treatment Options For Chronic Osteomyelitis

Diagnosis And Management Of Osteomyelitis American Family Physician

Bone Penetration Of Antibiotics Download Table

Diagnosis And Management Of Osteomyelitis American Family Physician

Diagnosis And Management Of Osteomyelitis American Family Physician

How To Spot Osteomyelitis Infographic Bone Infection Med Surg Nursing Pediatric Nursing

Diagnosis And Management Of Osteomyelitis American Family Physician

Diagnosis And Management Of Osteomyelitis American Family Physician

References In Osteomyelitis The Lancet

Current Concepts Of Osteomyelitis The American Journal Of Pathology

Risk Of Osteomyelitis With Joint Replacement
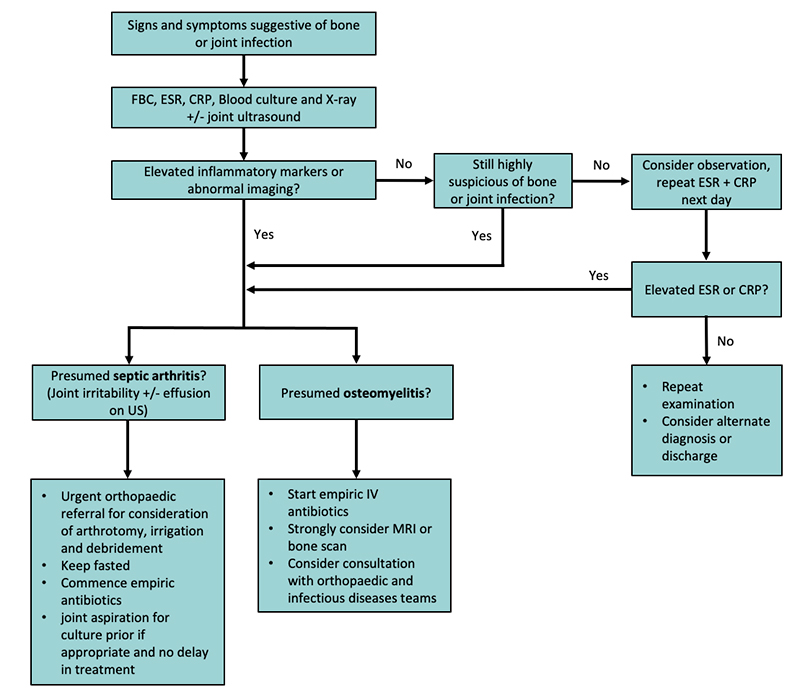
Clinical Practice Guidelines Bone And Joint Infection

Are Oral Antibiotics An Effective Alternative To Intravenous Antibiotics In Treatment Of Osteomyelitis Of The Jaw Journal Of Oral And Maxillofacial Surgery
/osteomyelitis-overview-4580405_Toxoplasmosis-5c6f2bb0c9e77c0001ddce61.png)
Osteomyelitis Symptoms Causes Diagnosis And More

Current Concepts Of Osteomyelitis The American Journal Of Pathology

Osteomyelitis Bone Infection Nabil Ebraheim Md Orthopedic Surgeon
Comments
Post a Comment